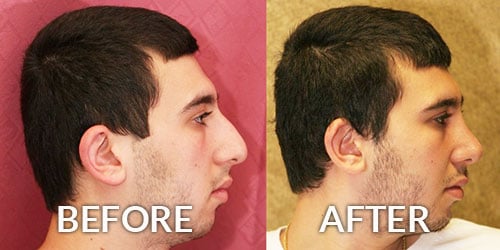
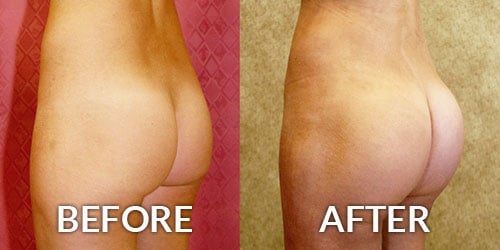
Functional Rhinoplasty – Correction of Nose Breathing
Consultations offered at our three convenient locations in Encino, Glendale and Bakersfield
We breathe, smell, and even taste with our nose!
The true function of your nose goes beyond just breathing, and its function is related to that of the sinuses, ear and the throat. When nasal passageways are obstructed, not only does breathing become difficult, but also the sinuses and the pressure balance of the ears are affected. That is why patients with chronic nasal airway obstruction also often suffer from chronic sinus and even ear infections.
Patients with nasal airway obstruction are often complaining of inability to breathe through one or both nostrils at night or during sports, post-nasal drip, dry mouth, sinus headaches, and pressure.
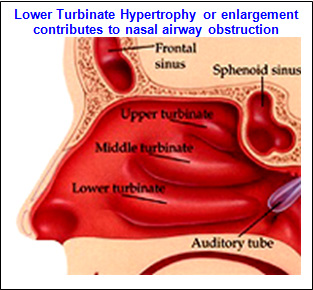
The next level of nasal airway obstruction occurs deeper and at the level of nasal septum and inferior turbinates. The nasal septum is a wall-like structure that divides the two nasal passageways. It is made of cartilage and bone that is covered in nasal mucosal lining. There are many people that are either born with a deviated nasal septum or develop it as a result of trauma or surgery. The combination of a deviated septum and enlarged inferior turbinates can severely obstruct the nasal airway. The septum can be straightened and the crooked parts removed in a procedure called Septoplasty. It is not uncommon to also harvest part of the nasal septum cartilage during a cosmetic Rhinoplasty to augment parts of the nasal skeleton.
The inferior turbinates are a pair of three levels of turbinates that help to humidify and regulate the flow of air. Either inherent enlargement and/or inflammation can result in significant enlargement of the inferior turbinates, thus blocking the nasal airway. This obstruction is alleviated by reducing the size of the inferior turbinates by a procedure call Turbinectomy. While some surgeons cut down part of the turbinates, others use electric cautery or radiofrequency energy to shrink them. Turbinectomy is a procedure that must be performed with the utmost care by a skilled surgeon who is highly experienced in the procedure, as the over removal of the turbinate can result in “Empty Nose Syndrome” (ENS). Symptoms of ENS include shortness of breath, chest tightness, breathing problems, abnormal heart rate, and the inability to control breathing. These symptoms are difficult to address as the turbinate tissue doesn’t regenerate.
In conjunction with these procedures the maxillary or frontal sinuses can also be assessed and cleaned through sinus endoscopy.
Nasal Injury Repair Surgery corrects injuries to nasal bones and the nasal septum when they are fractured or disrupted. The timing of this surgery is crucial as nasal bone fractures tend to heal quickly. As a rule, nasal Injury Repair Surgery is performed through a “closed” technique where skin incisions are not necessary. In those with very severe nasal skeletal collapse “open Rhinoplasty” will provide better access to the nasal skeleton.
Today, plastic surgeons can also restore “over-operated” areas by harvesting septal or ear cartilage and grafting it into a tiny pocket made inside the nose to correct certain deformities such as that of the bridge such as a “Saddle Nose Deformity”, or that of the tip via Tip Rhinoplasty.
Depending upon the patient’s needs, Tip Rhinoplasty can reduce or increase the size of the nasal tip, narrow the width of the nostrils, or change the angle between the nose and the upper lip. Tip Rhinoplasty can also help correct birth defects.