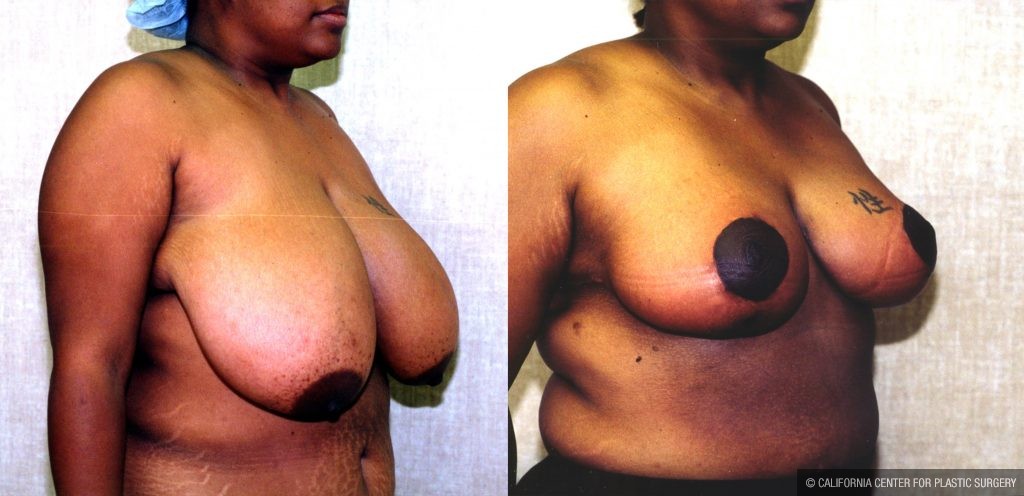
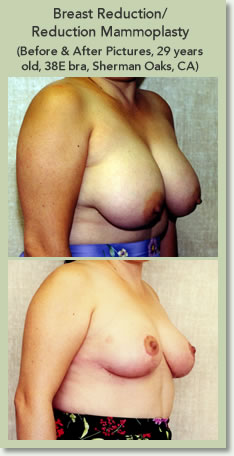
Breast Reduction (Female)
Consultations offered at our three convenient locations in Encino, Glendale and Bakersfield
For women with overly large breasts, performing even the most routine tasks can be a painful chore. Excessively large breasts put a lot of extra strain on a woman’s neck, back, and shoulders. The added weight on their bra straps can cause painful grooves on the shoulders, and chaffing is often a common occurrence. This is why breast reduction patients are often the happiest. Not only do they feel better about their appearance after surgery; they are also able to say goodbye to the physically painful burden of having large, heavy breasts.
Patients who undergo breast reduction surgery typically report relief from their pain. In addition, most are pleased to find they can now wear clothes that flatter their overall figure better. They also find that they can participate in physical activities like never before, and everyday tasks are easier.
Contents
- 1 Before and After Photos
- 2 The Procedure
- 3 Reason For Breast Reduction
- 4 Candidates
- 5 Preparations
- 6 Recovery
- 7 Will Insurance Cover the Cost of Breast Reduction Surgery?
- 8 Risks & Complications
- 9 FAQ
- 9.1 Will the Nipple-Areolar Complex be Detached?
- 9.2 Can a Breast Reduction Be Combined with Other Procedures?
- 9.3 What is the Nipple Pedicle Technique?
- 9.4 What Are the Advantages of the Nipple Pedicle Technique?
- 9.5 What Is the Free Nipple Graft Technique?
- 9.6 What is Scar-Less Breast Reduction?
- 9.7 I Am a Longtime Smoker. Will I Have to Quit?
- 9.8 How Long Will the Surgery Take?
- 9.9 How would you be evaluated for Reduction Mammoplasty?
- 9.10 Can I Have Breast Reduction Surgery if I Have Medical Conditions Besides Those Caused by Large Breasts?
- 9.11 Can I Have Breast Surgery if I Plan to Lose Much Weight After the Surgery?
- 9.12 How Soon After Childbirth Can I Have a Breast Reduction?
- 9.13 Are There Options Besides Surgery for Breast Reduction?
- 9.14 Is There A Minimum Age for Breast Reduction?
- 9.15 Is there an age limit for having Breast Reduction?
- 9.16 Does Breast Reduction Increase The Risk of Breast Cancer?
- 9.17 Does Breast Reduction Surgery Affect the Ability to Breastfeed?
- 9.18 How Will My New Breast Size Be Determined?
- 9.19 Will My Cosmetic Surgeon Show Me Pictures of How My New Breasts Will Look?
- 9.20 Will I Need a Mammogram Prior to Breast Reduction?
- 9.21 Can Males Undergo Breast Reduction?
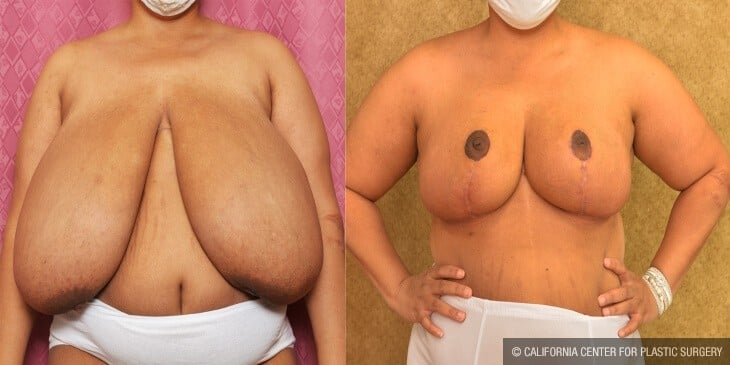
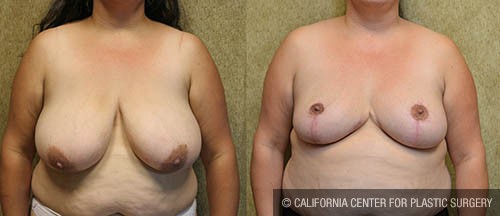
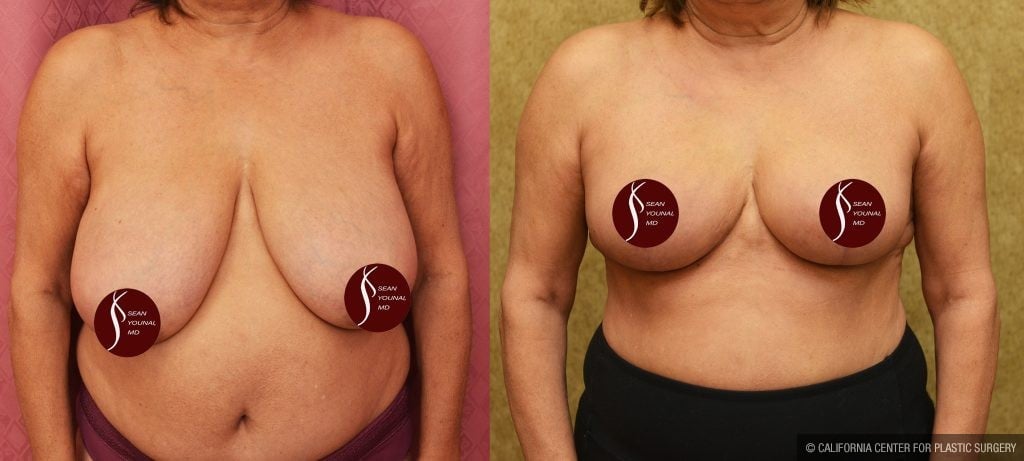
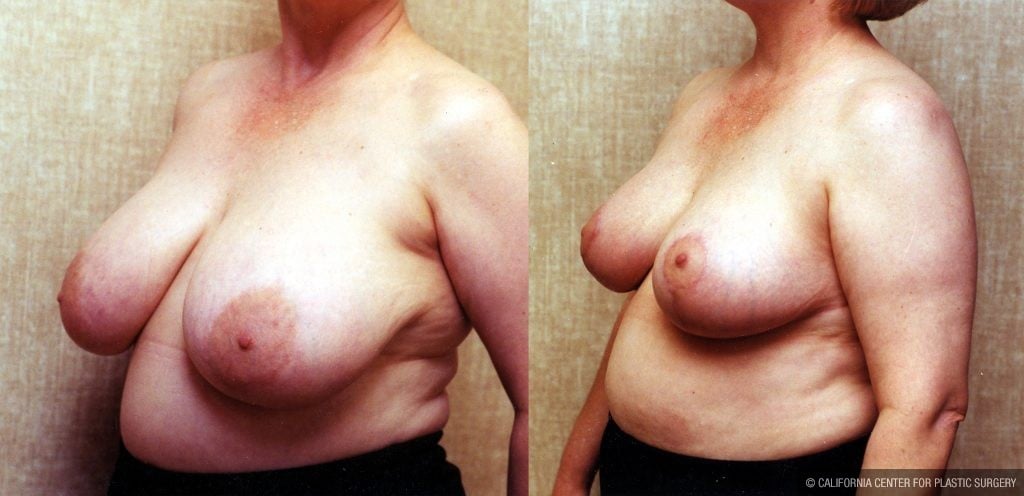
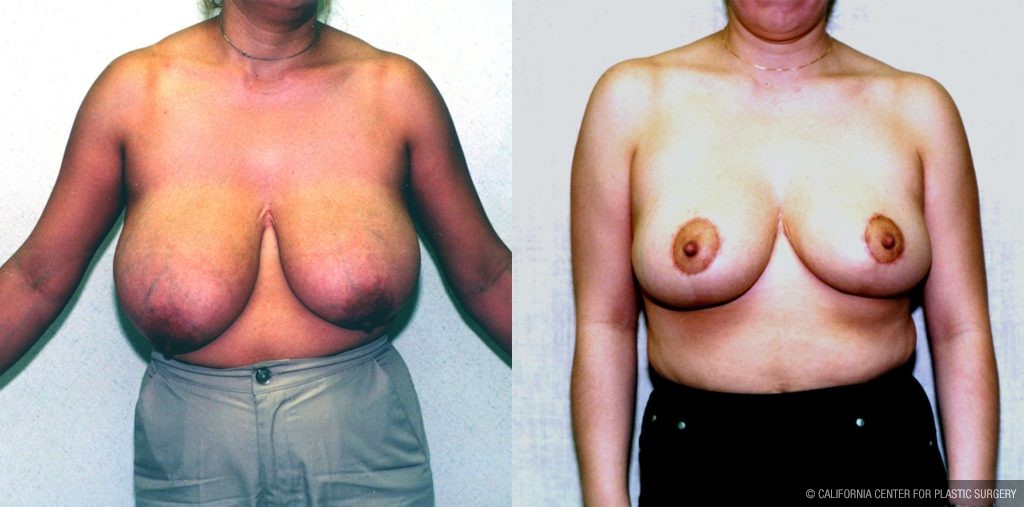
Before and After Photos
The Procedure
Breast Reduction, or Reduction Mammoplasty, is the surgical procedure to reduce breast size and weight through the removal of excess breast tissue, fat and skin. The plastic surgeon not only makes the breasts more proportionate to a woman’s figure, but also lifts them.
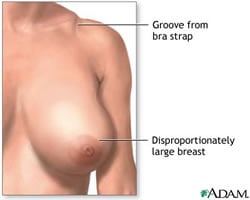
According to the American Society of Plastic Surgeons, 114,250 Breast Reduction surgeries were performed in 2005 on women who had excessively large breasts, a condition also known as Macromastia, Mammary Hypertrophy and Mammary Gigantism. Some girls develop breast overdevelopment (Mammary Hypertrophy) during puberty, while some women develop very large breasts (Gigantomastia) during pregnancy.
All of these women chose the option of Breast Reduction because it was the only way to correct the physical and emotional issues that are caused by excess breast weight.
Backaches, neck aches and hunchbacks. Rashes and skin irritation beneath breast folds. Painful grooves in the shoulders from heavy bra straps. Inability to exercise effectively or to participate in sports. Agony shopping for clothes that fit and look proportional. Unwanted attention!
These are just some of the torments that lead women with very large breasts to undergo Breast Reduction Surgery, or Reduction Mammoplasty. For many people, large breasts indicate femininity and beauty. This is not the case, however, for women who suffer the symptoms of having excessively large breasts, as described above.
Mammary Hypertrophy, or disproportionately large breasts, is indeed a disabling physical condition that is often overlooked in a culture that equates large breasts with attractiveness.
Large breasts – an ideal for many women – are nonetheless a source of pain, discomfort, and emotional trauma for many others. Women who suffer from overly large and disproportionate breasts (Mammary Hypertrophy or Macromastia) have felt embarrassment and shame from the time they reach puberty. They are distressed that their breasts, not their achievements or personality, are the first thing that people notice about them. Unlike their friends, they find it difficult to exercise, participate in sports, or to find bras and clothes that fit well.
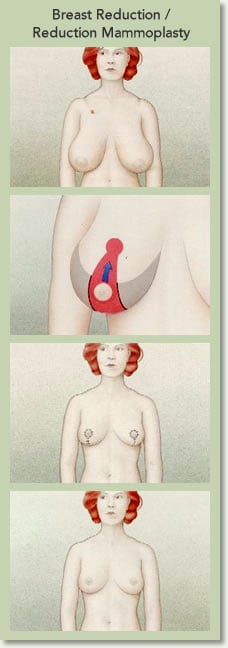
While some girls experience breast overdevelopment (mammary hypertrophy) during puberty, others develop gigantic breasts (Gigantomastia) during pregnancy. They suffer from chronic backaches, neck aches, painful indentations and grooves in their skin from heavy bra straps that cut their skin, fatigue, skin irritation (Dermatitis) and infection under their breast folds. All of this limits and constrains their lifestyle. In short, their breast size overshadows everything else in their lives.
According to the American Society of Plastic and Reconstructive Surgeons, the most common type of breast reduction surgery involves “an anchor-shaped incision that circles the areola, extends downward, and follows the natural curve of the crease beneath the breast.”
In summary, the surgery is generally performed by three incisions made by your cosmetic surgeon. One is made around the areola – the colored area around the nipple. A second incision is made vertically from the bottom of the areola to beneath the breast crease. A third incision curves in the under-breast (Inframammary) fold.
Breast reduction can be performed using many surgical techniques. The technique that is right for you will depend on your individual anatomy, including the size of your breasts and the amount of tissue being removed. The goals of breast reduction surgery are always the same, no matter what technique is used: reduce breast size, elevate the nipple, and make the areola smaller.
Dr. Younai typically performs breast reduction surgery using the inverted T or anchor-shaped incision method. This incision goes around the areola, extends vertically to the bottom of the breast, and then follows along the inframammary fold where the breast meets the chest wall. Excess skin and breast tissue is removed, while the nipple is repositioned higher up on the newly formed breast. The remaining skin is brought down around the areola to create the new breast contour.
The exact nature of your procedure may vary. For instance, women with the largest breasts usually benefit from the free nipple breast reduction technique, in which the nipple and areola are completely removed and relocated. Dr. Younai will discuss the details of your procedure during your consultation.
Reason For Breast Reduction
Chronic Pain
A woman with size “F” cup breasts is carrying approximately six pounds more than a woman with a “D” cup. This additional weight is sustained by the neck, back and shoulders, causing chronic pain in these areas. Many women find relief only through strong narcotics and muscle relaxants, leading to physical addiction, and emotional trauma. As such, Mammary Hypertrophy is a physical disability.
“I had disproportionately large breasts for so long; I was just accustomed to all of the symptoms — the back aches, the bad posture, the grooves in my shoulders. I can’t believe now that it didn’t even occur to me that I didn’t need to suffer all of those years. I only wish I had done this sooner. The relief is unbelievable.”
Lorraine, age 50
Disproportionate Breasts
Some women develop breasts that are disproportionate to their overall size, such as a petite woman with “D” cup breasts, who would be very “top heavy” and have difficulty finding clothes that fit properly.
Inability to Exercise
For many women with Mammary Hypertrophy, the mere weight of their breasts makes it impossible to maintain any kind of exercise routine.
Rashes And Infection
Excessive Sweating in the folds beneath large and pendulous breasts results in chronic dermatitis (skin irritation) and even fungal and bacterial skin infections in the inframammary fold. Furthermore, the wires in most support bras further irritate this area, resulting in long-term disintegration of the skin, and agonizing pain.
Breast Sagging
Often, women with large breasts have a pendulous breast shape, with nipples and areolas (the colored areas around the nipple) that point downward. Their heavy breasts sag so that they must always wear a bra and cannot wear revealing clothes.
Painful Shoulder Grooves
Painful and uncomfortable indentations result from the need to wear full support bras with tight straps, even to sleep.
Breast Asymmetry
Breasts with significant “unevenness” make women feel “lopsided” and make finding clothing difficult.
Insomnia
Many women with excessively large breasts have difficulty breathing during sleep, and often resort to sleeping upright while wearing their bras to bed.
Emotional Trauma
For many women, the discomfort and self-consciousness from excessive breast size becomes a problem that overshadows all other areas of their life – work, friendship and romance.
Some health plans cover Breast Reduction for chronic medical conditions, taking into consideration factors such as the amount of breast tissue to be removed, and how severe the medical, rather than cosmetic, problems are.
During the most common Breast Reduction surgery, the plastic surgeon makes an “anchor-shaped” incision the circles the areola, through a total of three incisions. One incision is made around the areola – the colored area around the nipple. A second incision is made vertically from the bottom of the areola to beneath the breast crease. A third incision curves in the under-breast (Inframammary) fold. The plastic surgeon then removes excess tissue, fat and skin, shifting the nipple and the areola into their new higher position. The plastic surgeon then brings the skin from both sides of the breast down around the areola, shaping the new contour of the breast. Skin that was above the nipple is lowered to the breast crease, allowing the surgeon to bring skin together and to reshape the breast.
Often, Breast Reduction is performed simultaneously with a Breast Lift or “Mastopexy,” because the excess fat and glandular tissue that made breasts large and heavy lead to sagging that can only be corrected by a lifting procedure. Men who develop excessively large breasts, or “woman-like” breasts – a condition known as Gynecomastia – can also undergo Breast Reduction.
Breast Reduction is a very technically challenging procedure that should be performed only by a board-certified plastic and reconstructive surgeon who is highly experienced in performing it.
Candidates
Who Is Not A Good Candidate
Women who do not have disproportionately large breasts – a “D” cup or larger – or who do not suffer from the above noted symptoms of large breasts are not good candidates for Breast Reduction. You shouldn’t undergo a breast reduction if you don’t have large breasts and just want to have your breasts lifted. Instead you should undergo Mastopexy, or a Breast Lift. Also, if you are planning another pregnancy, you should postpone Breast Reduction surgery. Your ability to breast feed can be reduced by this surgery. In addition, women who are in the process of losing weight should delay their reduction mammoplasty until their weight has stabilized.
Is It Hereditary?
While this is often the case, it is not always true. For example, some women who had a relatively small breast size before pregnancy experience a dramatic and uncomfortable increase in their breast size following childbirth.
Preparations

The surgeon will provide very specific instructions prior to surgery so you will have an optimal and safe experience. These include what medications to avoid to prevent excessive bleeding and bruising, required medical exams, what to eat and drink prior to surgery, and the prescription of an anti-nausea pill to take on the morning of the surgery.
In all cases, you will be asked to have a reliable friend or family member take you home after the surgery, as you will not be allowed to drive.
- Tend to all of your chores and to do things before your surgery so you don’t have to worry about taking care of things early during your recuperation. You are not allowed to engage in heavy lifting for several weeks after surgery. This means if you usually clean the house, you should do so in advance of your surgery.
- Have your hair cut and colored, wax your legs, pay your bills, and take your dog to the vet before your planned day of surgery!
- If you an avid tanner, don’t tan your breasts for one week before, and six weeks after, your surgery. Any sun or tan burn of your breast skin can potentially increase the risk of infection of skin damage with breast augmentation.
- If you have nipple rings you must replace them with a plastic ring at least one week before surgery and wait for your surgeon to tell you when you can have them replaced.
- Rent your favorite movies, and leave easily prepared foods and snacks in areas where you will not have to lift or reach.
- Place all of the medications, tissues, reading materials, water bottles on one table, within easy reach.
- Have ice cold cola drinks, ginger ale, or sport drinks close to your bed. Avoid drinking too much plain water after surgery, because it makes you more nauseated.
- After surgery take your nausea pill about one hour before your other medications to lessen nausea. Also, have some over-the-counter anti-acids available at your bedside.
- Some surgeons recommend putting cold packs on you breasts afterwards. In my opinion, even though cold might lessen the inflammation, it can also cause frostbites or skin damage while your breasts are numb after surgery.
- Pain Pump is a relatively new device used to deliver anesthetic solution into the breast tissue during the first 48 hours after surgery. It is the size of a Walkman radio that is connected to breast via two very thin catheters that deliver the anesthetic solution. This machine reduces but does not eliminate the need for taking oral narcotics. Patients who are very sensitive to pain or who cannot tolerate oral narcotics find this device very useful. Others feel that it is cumbersome because that it is attached to your breasts for two days.
- Arnica Montana or Bromelain homeopathic herbs have been used in Europe for centuries to treat swelling, soreness and bruising. When properly prepared, Arnica may significantly decrease the healing time or the appearance of such. There are many formulations from different companies. Sublingual (under the tongue) types are the most often recommended for plastic surgery. I have seen variable results with its use. There are some patients that did not benefit from it and other who appeared to benefit. Therefore, I am open to its use if a patient would like to use it.
Pre-Operative Checklist

- If you are older than 45 years, or have heart disease, we require a pre-operative EKG, which would either be done by your internist, cardiologist, or at our facility. Heart disease and all other medical illnesses need to be optimized by, and you be cleared by an internist or specialist prior to surgery.
- Pre-operative laboratory blood and urine tests are done usually within 10 days of your surgery date. If you do have health insurance this might be covered, otherwise, the laboratory will charge you.
- If you have specific medical illnesses, allergies, or physical handicaps, please notify our staff during your pre-operative visit.
- Please refrain from taking any Aspirin, Aleve, Advil, Motrin or other NSAID for ten days prior to your surgery. These drugs can increase the incidence of bleeding and bruising.
- Do not drink or eat after midnight on the night before your surgery. This means no coffee or breakfast in the morning of your surgery. You should take all of your medications with a little water.
- Please remove and leave behind all jewelry, watches, and body rings before you come in for your surgery. Please do not wear any makeup, body lotion, or perfume.
- Before leaving home for your surgery, take one “nausea pill” — COMPAZINE — with a little water.
- Please wear comfortable and loose clothing the day of surgery. It would be helpful if you wear front open tops and loose sweatpants.
- If you have long hair wear a non-metallic cloth ponytail.
- Do not wear very dark nail polish.
- You should make arrangements for a friend or family member to take you home after surgery. You are not allowed to drive yourself home or take a taxi.
Recovery
Recovery from breast reduction surgery can take several months. Although many women are able to return to work in just two weeks, more strenuous activity will need to be held off for much longer. Dr. Younai will help guide you through every step of the recovery process to ensure your comfort and safety. It usually takes several months before your breasts settle into their new, permanent shape.
Dos and Don’ts

Breast Reduction surgery generally takes between four to six hours, as an outpatient surgery. Afterwards, you will spend some time in the Recovery Room of the surgical facility. When you wake up, you will have gauze dressing over your breasts, and a support bra. You will also have drains that leave the skin at the outer sides of your breasts. The nurse and/or the doctor will give you and your family drain-care instructions.
Do not be alarmed if you feel discomfort from bruising and swelling. This is a normal result of the surgery, particularly for the first 48 hours. Your cosmetic surgeon will prescribe medications to relieve this discomfort.
At your first office visit following surgery, the bandages or surgical bra will be replaced with a softer support bra, which you will wear all of the time, day and night, for three to four weeks. These will help your breasts to retain their new shape.
There would be no sutures to be removed. The Steristrips that are applied to your incisions will either fall off in about three week or you can gently remove them by then.
Your cosmetic surgeon will provide you with specific instructions for your recovery, including what medications to take and how to limit your activities.
“Over time, the woman who always felt bad about her body morphed into someone who…well, just stopped thinking about how miserable it made her feel. It took a period of adjustment; then I just adopted the new me and I feel great about it. I feel freed of a great burden.”
Sandy, age 45
Post-Operative Instructions
- You will have some pain and nausea after your surgery. Your physician will prescribe the appropriate antibiotics and pain medications.
- For the first two to three days, sleep with your head elevated.
- Do not sleep on your stomach or sides until cleared by your physician.
- Do not remove your bandages until instructed to do so by your physician.
- Do not drink alcohol, take aspirin, or diet pills until your physician gives you approval to do so.
- Refrain from smoking for at least two weeks.
- Wear soft bras or maternity bras with NO under wire for at least six months after your surgery.
- You may walk, but you cannot participate in sports or strenuous physical activities until cleared by your physician.
- Do not raise your arms above your head for two weeks. This can potentially cause a displacement of your implants.
- Keep your drains in a position where they will not attach to anything and be accidentally removed. Keep a log of how much fluid is drained, twice daily. Usually, when the total volume of drainages subsides to less than 30 ccs per day, the drains will be removed by the nurse or the doctor.
- Areas of your breasts or nipples will be numb for several weeks after surgery. This is normal and expected.
- The day of your surgery, wear loose, comfortable clothing that opens in the front, such as a jogging suit. Wear shirts that button down the front, and don’t need to be put over your head.
- If you have any important or urgent questions within the first week after surgery, you are welcome to call our office at any time.
Tips for Your Significant Others

The support of your family and loved ones can be as important to your healing as following your physician’s medical directives. Their understanding of the pain, discomfort, and at times, the roller coaster of emotions that you might experience can make all the difference in having an optimal outcome.
Here are some tips for your significant others that will be helpful to them in helping you:
- You should be available as a full time caregiver for at least 48-72 hours to help the patients with the tasks that are normally taken for granted, like being able to walk to the bathroom.
- You, or someone, should care for the patient’s children for a minimum of two to four days, and be sure that she has assistance in lifting young children for several days after your surgery.
- Help with pet care. Someone should walk them, feed them and clean up after them for at least several days.
- Prepare to help the patient address the swelling that she will experience, according to her physician’s instructions. This may include ice packs or gel pack specifically designed for breast surgery patients.
- Know that she may experience mood swings and feel like crying off and on – especially in the first couple of weeks. This is a normal aftermath of major surgery.
- Encourage her to drink lots of water – to address bloating and to keep her hydrated.
- Remind her to not fight the pain – she should go with the flow, and take her medications as directed. It is not good to try and be a hero!
- Have her use a U-shaped pillow for sleeping and resting.
- Give her lots of compliments. She may be fearful because it will take some time before her new breasts appear as they should. She has a lot of healing to do!
- Prepare simple and easily digestible foods, such as scrambled eggs or Jell-O.
- Remind her to sleep on her back!
- Have two sleep-in bras at the ready – one tight and one loose to alternate as needed.
- Be there when she goes to have her bandages removed, to support her through any discomfort she may be feeling.
- As far as sex is concerned, let her initiate things and play it by ear.
- Some women are fearful that they might harm their implants if they are touched or manipulated after surgery. Have them ask their doctor about this and get some reassurance.
- Some women feel depressed or regretful about having undergone breast surgery. Sometimes they don’t know how to handle the attention or questions that breast surgery will bring about. At the same time, significant others can develop uneasy feeling about the fact that you underwent such surgery. It is good to talk about your feelings and to even seek outside help if you can’t resolve some ambiguities.
Recovery Time
Relief from neck and back strain is immediate for most women. Full healing can take a year or more, and generally it takes several months for your breasts to take on their final shape.
“I can’t believe how much easier shopping for clothes is now. Before my reduction, I had to buy separates – with a huge difference in sizes. Now, I can actually wear a dress! I can stand straight and the pain in my shoulders is gone. My one and only regret is that I waited so long to do this.” — Mary, age 50
Immediately after surgery, breasts look rather flat and wide. Within several weeks they look like cones or “torpedo” sticking straight out. This is because the skin envelope is tightened over the breast tissue, and it takes several months for the breast skin to stretch and the breast tissue to settle into its final form.
However, after three to six months, most women find that their breasts are smaller, firmer, and with a natural look and feel.
Because of how quickly Breast Reduction resolves medical symptoms, it is often described as the surgery that results in the most dramatic change in your body image. As such, be prepared for friends, family – and yourself – to need time for adjustment!
Will the Results Be Long Lasting?
For most women, the results are long lasting, except for women who lose a lot of weight or become pregnant. As is the case for all women, however, aging and gravity take their toll, and may eventually affect your outcome. Down the road, some women opt for a Breast Lift, or “Mastopexy,” to retain their new look.
Bra Sizing

It is imperative that you wear a proper fitting bra. If not, you will eventually have breasts that sag, back aches, shoulder aches, thinning skin and other problems. Many believe in formulas which determine your exact bra size, and while this can help and start you on the right path, it is most certainly individual. Try on a bra and wear it for a while and you will know if it is too large for you. Finding the perfect bra isn’t impossible after your surgery, it just may be a little more difficult. But all in all, it is very important to find one that properly fits your frame and supports your breasts.
- If your bra band is riding up in the back and if you find yourself trying to lift your breasts by shortening your shoulder straps you are only doing your breasts a disservice.
- Also very important, when buying a new bra, it should fit snugly on the last setting (the loosest hook set) this way when your bra stretches with wear you can fasten it tighter if needed on the next two settings.
- If you find post-operatively that your bras bag at the nipple area, try purchasing a bra with Lycra in it. This helps the bra to conform to the breasts.
- If you have that horrible quadruple-boob look, where you look like your breasts have been split in two and have that not so appealing double-decker appearance, you need a larger cup size.
- Do your breasts fall out when you bend over? You may need more coverage.
- Bra Care: It is best to either hand wash and line dry your bras, or machine wash inside of a lingerie bag. Then line dry to extend the life of your bras. High heat will weaken elastic and ruin your bras.
- Be sure to re-measure yourself in the event of weight gain or loss — even if 7 to 10 lbs. — pregnancy, or simply as time goes by. Measurements can vary over the years.
Will Insurance Cover the Cost of Breast Reduction Surgery?
Most women who undergo breast reduction surgery are able to get the costs covered by their insurance companies. Because of the physical pain caused by overly large breasts, breast reduction is usually considered a medical procedure. Your coverage may vary. However, we are here to help you navigate the details of your policy. In fact, we deal with insurance companies almost daily and know exactly what is required.
“It took some time to get my insurance company to approve this surgery, even though the pain from having large breasts is as real as the pain of any other chronic disease. Once they approved the cost of this surgery, it took about six weeks until I could actually undergo it. After living like this all of my life, the waiting seemed like forever. But it was well worth it.” — mdash; Mary, age 41
Because disproportionately large breasts lead to a number of chronic medical conditions, such as severe back pain, many health plans will cover the cost of Breast Reduction surgery. Insurance companies will consider factors such as the amount of breast tissue to be removed, what kind of coverage you have and how severe the medical complications from your breast size are. In other words, their focus is upon medical, rather than cosmetic, necessity. The companies may require that a certain number of “grams” be removed from the breasts for the surgery to be considered medically necessary.
In general, most insurance companies require that you have had at least six months of documented evaluations and treatments by your primary care physician in order to rule out spinal disorder as the primary cause of your neck and back pain. You must have undergone six months of physical therapy and other conservative treatments of your back and neck pain and have recommendations from both your primary doctor and your physical therapist, spine surgeon, or chiropractor that you will benefit from reduction mammoplasty.
Some insurance companies do require photographic documentation of your breast size as well as a complete letter delineating all your symptoms that have risen from this disease. Finally they require that a large portion of breast tissue (minimum 500grams, 1.2 lbs.) be removed from each breast in order for this surgery to be considered medically necessary and not just as a mean of getting a Breast Lift.
The following is an example from The Regency Blue Cross Group’s listed Policy and Criteria for determining a Breast Reduction as Medically Necessary.
Policy/Criteria
Reduction mammoplasty may be considered medically necessary when two or more of the following clinical indications and physical findings are present, which have failed to respond to appropriate conservative therapy:

- Documented pain in the upper back, neck, shoulders, and/or arms, which must be of long-standing duration and increasing intensity
- Ulceration of the skin of the shoulder or shoulder grooving
- Intertrigo between the pendulous breasts and the chest wall
- Lordotic posture
- Ulnar paresthesia
In addition to the above clinical indications, the following criteria must also be met:
- The patient must be old enough that the breasts are fully grown; and
- The amount of breast tissue removed from each breast must be either:
- A minimum of 600 grams or
- If less than 600 grams is to be removed, then the tissue removed must be equal to or greater than the 22nd percentile cutoff weight for body surface area* (see below for body surface area/breast weight table).
- In cases of significant asymmetry (i.e., one breast meets criteria A or B above, but the other breast does not), the total amount of tissue removed for both breasts must be equal to or greater than two times the minimum as determined in A or B above. For example, if the criteria require removal of 500 grams per breast, a total of 1,000 grams must be removed. 400 grams may be removed from one breast as long as 600 or more grams are removed from the second breast.
Risks & Complications
What Are the Risks and Complications of Reduction Mammoplasty?
As with any major surgery, your risks are higher if you have diabetes, poor circulation, heart, lung or liver disease, if you are a smoker or have a family history of blood clots. Your cosmetic surgeon will want to assure that any medical conditions have been treated, and optimized, before you can consider having a Breast Reduction.
Infection
The risk of wound infection is less than two percent. Most patients receive intravenous antibiotics during surgery and antibiotic medication after surgery, which minimizes this risk. Sometimes accumulated of blood (hematoma or seroma) can become infected, requiring drainage and further coarse of antibiotics. In extremely rare instances, life-threatening infections, including toxic shock syndrome have been noted after breast surgery. Individuals with an active infection in their body or weakened immune system should not undergo breast surgery.
Bleeding
While this is unusual, it is possible to experience a bleeding episode following surgery. If this occurs, emergency treatment to drain accumulated blood, or a blood transfusion, may be required. You can reduce this risk by not taking any aspirin or anti-inflammatory medications for ten days before or after surgery. Non-prescription “herbs” and dietary supplements can also increase the risk of bleeding. The risk of major bleeding, or blood collection, is only about three percent. Most women lose about two test tubes of blood during surgery. Any blood clots that form must be removed in a later surgical procedure.
Hematoma & Seroma Pain
Sometimes blood in the depth of the breast tissue can accumulate and form a blood collection, called a Hematoma. Seroma is a fluid that arises from the breakdown of accumulated blood or Hematoma. In cases with extensive dissection and manipulation of the breast tissues, most plastic surgeons place a drain in the depth of the breasts to remove accumulated blood and fluid and thus prevent formation of a seroma. After drains are removed, this fluid may re-accumulate in the breasts, especially following trauma or vigorous exercise. Additional treatment may be necessary to drain the accumulation of fluid from the breast.
As is the case with any major surgery, a Breast Reduction involves pain. Most women say that the pain is greatest in the first 48 hours after surgery. However, this will be minimized by the prescription that your cosmetic surgeon will prescribe before you go home. In very rare cases there are some women that develop chronic or long-term pain that will require further treatment.
Scarring
All surgeries of the breast involve some scarring, which is permanent but will fade with time. People scar differently, and some women are more delicate than others. All scars appear red and lumpy at first. Also, some ethnic groups are prone to the formation of thicker scars. Your pattern of scarring in the past could be a good predictor of how you will scar following a Breast Reduction. In most women, the scars will be less noticeable within one year. In rare cases, scars may require surgical revision or treatment. Poor healing and scarring are more common in smokers.
As a rule, your cosmetic surgeon will place incisions in areas that can be covered by a bathing suit or under garments.
Change in Nipple and Skin Sensation
After breast surgery, it is normal to experience temporary numbness of the skin and the nipples. This usually resolves from six weeks to six months. During this period, you may even experience a period of increased sensation or hypersensitivity that can be treated with massage. Permanent partial or complete loss of nipple and skin sensation can occur following a Breast Reduction in one or both nipples. This can depend on the extent of breast surgery. However, since the plastic surgeon doesn’t detach or remove breast tissue, nipple sensation is usually preserved. In general, the incidences of partial or complete loss of nipple sensation are each about 10%.
Asymmetry

As is true in nature, no two breasts are identical. This is even more common with sagging breasts. After Breast Reduction surgery, there is a period of healing and settling of the breasts. During this period breasts with different extent of sagging and laxity will settle at different rates. Therefore, it is very common to see some differences early on during the healing period. Afterwards, there may appear some slight differences between your breasts, but it should be no more pronounced than that which would happen in breasts naturally. In some cases, additional surgery may be performed to improve symmetry.
Fat Necrosis
There is a risk that small areas of fatty tissue deep within the breast might die. Sometimes, this causes hardness within that area of the breast that may be mistaken to be breast lumps. Mammogram can help differentiate between the two. In some cases, removal of fat necrosis through surgery may be necessary. Smokers have an increased risk of skin loss and wound healing.
Delayed Healing
Wound disruption or delayed wound healing is possible. Some areas of the breast skin or nipple region may not heal normally and may take longer to heal. This is especially common at the junction of the Inverted-T incision. Usually, these will heal without any sequel over several weeks.
Areas of skin or nipple tissue may die. This may require frequent dressing changes or further surgery to remove the non-healed tissue. Individuals who have decreased blood supply to breast tissue from past surgery or radiation therapy may be at increased risk for wound healing and poor surgical outcome. Smokers have a greater risk of skin loss and wound healing complications.
Sutures
Most surgical techniques use deep sutures. You may notice these sutures after your surgery. Sutures may spontaneously break through the skin, become visible or produce irritation that requires suture removal.
Nipple-Areola size and shape
Following Breast Reduction, the size, shape, and position of the nipples will not be identical as it is true in normal breasts. Depending on the skin elasticity of the two breasts, one areola might stretch more than the other after a surgery.
Recurrent Ptosis

The breast skin and tissue continue to change with age, with gradual loss of its elasticity. Breasts continue to age and sag with time even after surgery. Those who have breasts with sun damaged thin skin and stretch marks, or those after weight loss, or with inherently poor elasticity are at a higher risk of developing recurrent sagging (ptosis) early on. In this group there is also a relatively high incidence of “bottoming out” of the breasts. Under this circumstance the weight of the breast tissue can stretch out the lower breast skin causing the majority of the breast tissue slides below the level of the nipple, making it appear that the nipple is sitting too high on the breast.
Skin Discoloration/Swelling
Bruising and swelling normally occurs after a Breast Reduction. The skin in or near the surgical site can appear either lighter or darker than the surrounding skin. It is very rare, however, for swelling and skin discoloration to be permanent.
Allergic Reactions
In rare cases, patients may experience allergies to tape, suture material and glues, blood products, topical preparations or injected agents. Sometimes these reactions also, rarely, include systemic reactions such as shock from drugs used during surgery and prescription medicines.
Anesthesia Reactions
All anesthesia, local or general, involves a risk of complications, injury and even death. You should interview your cosmetic surgeon thoroughly about the kind of anesthetist that he or she employs. While many surgeons use nurse anesthetists, the safest option is a physician who specializes in anesthesia. This is particularly true when the surgery is performed in a surgical facility other than a hospital. A physician anesthetist is better qualified to address any complications that may arise.
Future Pregnancy and Breast Feeding
It is possible that pregnancy will cause your breasts to enlarge and your breast skin to stretch. Therefore, it can offset the Breast Reduction results.
As a general rule a Breast Reduction or any breast surgery that involves rearrangement of the breast tissue can affect a woman’s ability to breast feed. Because during breast reduction the nipple is generally not detached or separated from the milk glands, there is a reasonable chance of preserving breast feeding ability.
Emotional Changes
Your cosmetic surgeon will advise you that the change may feel very dramatic to you, and you may need some time to adjust to your new look. In many cases, however, the almost immediate relief from medical problems and the emotional traumas that accompany overly large breasts is a source of happiness for patients. The level of patient satisfaction from Breast Reduction surgery is among the highest of all plastic surgery procedures.
FAQ
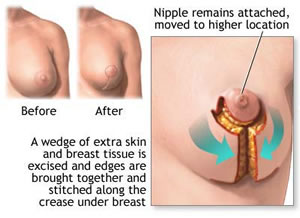
Will the Nipple-Areolar Complex be Detached?
As a rule, the nipple-areolar complex remains attached to its blood vessels and nerves. While attached to its roots, it is gently moved up to a higher position on the breast in order to correct sagging. Under this circumstance, the sensation of the nipples is mostly preserved.
However, if a woman has especially large or pendulous breasts, the nipples or areolas may have to be completely removed and grafted into a higher position – with a subsequent loss of sensation in the nipple and areolar area. Sometimes the areola will be reduced in size.
Can a Breast Reduction Be Combined with Other Procedures?
Your cosmetic surgeon will determine, based upon your medical history and needs, how many procedures can be done simultaneously. However, often Breast Reduction is performed simultaneously with a Breast Lift, or “Mastopexy.” This is to address the sagging skin that has been caused by the weight of large breasts over the years.
Many women need a Breast Lift in combination with a Breast Reduction. Because of the volume of excess fat and glandular tissue that made breasts large and heavy, the patient’s sagging is often not fully corrected. A Breast Lift places the smaller breasts higher up on the chest for a perkier and more youthful outcome.
Liposuction is another procedure that may be combined with Breast Reduction. Often, women with Mammary Hypertrophy have excess fat and bulging in their lateral chest wall, which is not contained by their bras. This area can be liposuctioned at the time of a Breast Reduction to further contour a woman’s upper body.


What is the Nipple Pedicle Technique?
The most common type of Breast Reduction utilizes a nipple pedicle technique that keeps the nipple-areolar complex attached to its deep blood supply pedicle, or to a superior pedicle of skin. Through this technique, the nipple-areolar complex is raised to a higher position, while leaving it attached to portions of the underlying breast tissue for nourishment. Areas of surrounding skin and breast tissue are then removed to create a smaller breast. Remaining skin and breast tissue is then wrapped around the nipple-areolar complex in its new location.
What Are the Advantages of the Nipple Pedicle Technique?
One advantage is a lower rate of nipple loss. Another is that the nipples usually maintain their color and sensitivity. Also, many cosmetic surgeons believe this produces the most aesthetically pleasing outcome.
A disadvantage of this technique is that it is technically more challenging in women with very large cup sizes (E or larger), or very pendulous breasts, because they are more likely to have problems with nipple loss or loss of nipple circulation. However, in my practice, I have been able to utilize this technique very effectively even in women with very large breasts in order to help preserve their nipple sensation.
What Is the Free Nipple Graft Technique?
With the Free Nipple Graft Technique, the nipple-areolar complex is first completely detached and removed, and preserved for later in the operation. After the removal of excess breast tissue and skin, the remaining tissues are reassembled to form the new breast shape. Trimmed to a smaller size, the nipple-areolar complex is sewn onto the breast as a skin graft.
Because this procedure is faster, it is recommended for elderly women, women with major medical problems and for women where very large amounts of tissue will be removed. Disadvantages of this surgery include the loss of nipple sensation, inability to breast feed, and a flattened looking nipple-areolar complex.
What is Scar-Less Breast Reduction?
Besides the conventional Breast Reduction, which involves actually removing segments of the breast tissue and skin, the volume of the breast can also be reduced with Liposuction. The utility of liposuction for breast reduction, also called “Scar-Less Breast Reduction” is limited. First, only excess fat and not the breast gland can be removed. Second, excess skin cannot be removed which can potentially lead to breast sagging. Third, it is difficult to evaluate the removed fatty liquid for evidence of breast cancer. Finally, the resulting scarring from liposuction can potentially hinder adequate assessment of breast lumps during mammography. Therefore, liposuction is used selectively in those who don’t need large reductions of breast volume, and who have very tight and elastic skin with no concurrent sagging.
I Am a Longtime Smoker. Will I Have to Quit?
Stopping smoking will greatly reduce your risk of surgical complications, and of complications during healing. Nicotine chokes blood vessels that feed the nipple-areolar complex, putting a patient at great risk of losing their nipple and parts of their breast skin after surgery. Therefore, almost all cosmetic surgeons will demand that you refrain from smoking for at least some weeks before, and after, your surgery.
How Long Will the Surgery Take?
Breast Reduction is a delicate and complex procedure that can take from 3-6 hours depending on the size of the breasts and the amount of lifting that is necessary.
At your consultation Dr. Younai will review your treatment options for Breast Reduction, including pros and cons of each procedure, potential risks and complications, recovery course, pre and post operative instructions, and esthetic outcomes. There are also many before-and-after pictures and high resolution images of Reduction Mammoplasty available in our photo gallery.
How would you be evaluated for Reduction Mammoplasty?
Your cosmetic surgeon will evaluate a number of factors at your first appointment. These include your measurements, the size and shape of your breasts, and the placement of the nipples and areolas. He or she will also take photographs so an accurate record of your progress can be kept. Your plastic surgeon will also give you an estimate of how much breast weight that can be removed.
Can I Have Breast Reduction Surgery if I Have Medical Conditions Besides Those Caused by Large Breasts?
Yes. However, your cosmetic surgeon will first require that your medical conditions, such as diabetes or hypertension, be optimized prior to your surgery. Uncontrolled diabetes, thyroid, and immune disease can complicate your healing after surgery.
Can I Have Breast Surgery if I Plan to Lose Much Weight After the Surgery?
You should postpone Breast Reduction surgery until you have lost weight and your breasts size and weight have stabilized. Excessive weight loss after reduction mammoplasty can cause dramatic sagging of your breasts, requiring further surgery.
How Soon After Childbirth Can I Have a Breast Reduction?
You cannot undergo general anesthesia, or take any medications, while you are breast feeding. Also, it takes about six weeks for your breasts to reach their stable size and weight after you stop breast feeding. After this, you may undergo Breast Reduction. However, make sure that you are not planning further pregnancies in the near future.
Are There Options Besides Surgery for Breast Reduction?
Obese women who have large breasts may consider losing weight before embarking upon Breast Reduction. This initial weight loss will first reduce their risk for surgical complications; second it will make their recuperation easier, and third will bring their breasts to their stable weight and size before proceeding with reduction Mammoplasty. Also, women who have back and neck pain along with large breasts should first try physical therapy and weight loss before considering surgery.
Is There A Minimum Age for Breast Reduction?
It is recommended that you don’t have breast surgery until you have reached adulthood and until after your breasts have stopped growing. Exceptions may be made for girls who have a rare and extreme kind of breast overgrowth known as “virginal hypertrophy.” These girls develop gigantic breasts during adolescence that become a physical and psychological predicament for them. After having undergone reduction mammoplasty during adolescence, these girls often have further Breast Reduction surgery at a later age when their breast size stabilizes.
Is there an age limit for having Breast Reduction?
Breast Reduction is not restricted to young women – elderly women may also be candidates for the procedure. Women from their teens to their eighties may undergo the procedure. Many women do wait until after age 50 to undergo the procedure – later lamenting that they didn’t do so sooner after a lifetime of the pain, rashes, back and posture problems.
Women undergo the procedure at different ages for different reasons. For example, some girls in their late teens realize they will not be able to endure a lifetime of the side effects of having large, pendulous breasts. Others may choose to wait until they have completed childbearing and breastfeeding before they seek the relief of Breast Reduction. Still others don’t act until referred by their general physicians to address neck and back pain.
Does Breast Reduction Increase The Risk of Breast Cancer?
Absolutely not! In fact, Breast Reduction reduces a woman’s chance for developing breast cancer. By reducing the total size of the breast, it reduces the area in which breast cancer can potentially develop. It also makes breast self-examination and mammography easier.
Does Breast Reduction Surgery Affect the Ability to Breastfeed?
As a rule, Breast Reduction will reduce your ability to breast feed. However, this can depend on the type of Breast Reduction that is performed. This will definitely be the case where the areola and nipple have been detached and grafted back onto the breast.
With the “nipple pedicle” technique, the nipple-areolar complex is kept attached to its roots, therefore lessening the chance of damage to the milk ducts. But even with this technique you can lose your ability to breast feed because a considerable amount of glandular breast tissue has been removed.
How Will My New Breast Size Be Determined?
Your cosmetic surgeon will take your measurements and discuss your options for a breast size that is both to your liking, and proportionate to your body frame. Many women feel like they want to go as small as possible, just to finally be rid of the large breasts that have hindered them for so many years. In the end, however, your cosmetic surgeon will discuss what size is realistic for you, to achieve the relief that you seek, while achieving the figure that is right for you.
Will My Cosmetic Surgeon Show Me Pictures of How My New Breasts Will Look?
Although no plastic surgeon can guarantee an exact bra size or breast shape, he or she can give you some indication of the range. They can also show you before-and-after pictures of women similar to you who have had reduction mammoplasty. You should also know that your chest frame places constraints on your surgeon with respect to the ultimate size and shape of your breasts.
Will I Need a Mammogram Prior to Breast Reduction?
Yes. Your cosmetic surgeon may recommend a “screening” mammogram prior to your surgery, depending upon your age, or family history of breast cancer. This will help detect questionable breast areas that can possibly be evaluated or biopsied at the time of your Breast Reduction surgery.
You will also be asked to have another mammogram several months following your surgery as a “baseline” for future mammograms. Additionally, breast exams and mammography may be easier to perform following Breast Reduction. Smaller lumps may be harder to detect in women with very small lesions but will appear more readily once the breast size has been reduced.
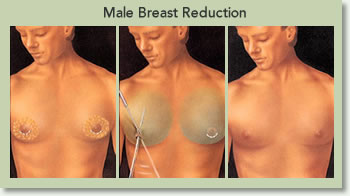
Can Males Undergo Breast Reduction?
Yes. Men like women can also develop disproportionately large breasts. This condition is called Gynecomastia –from the Greek words for “women-like breasts.” Development of breast tissue in men is actually quite common. Gynecomastia affects an estimated 40 to 60 percent of men. It may affect only one or both breasts. Although certain drugs and medical problems have been linked with male breast overdevelopment, there is no known cause in the vast majority of cases. In fact, one out of every three adolescent males develop significant breast tissue. Of these, one third will continue to keep their breasts into adulthood.
For men who feel self-conscious about their appearance, Male Breast Reduction Surgery can help. The procedure removes fat and or glandular tissue from breasts and in extreme cases removes excess skin, resulting in a chest that is flatter, firmer, and better contoured.