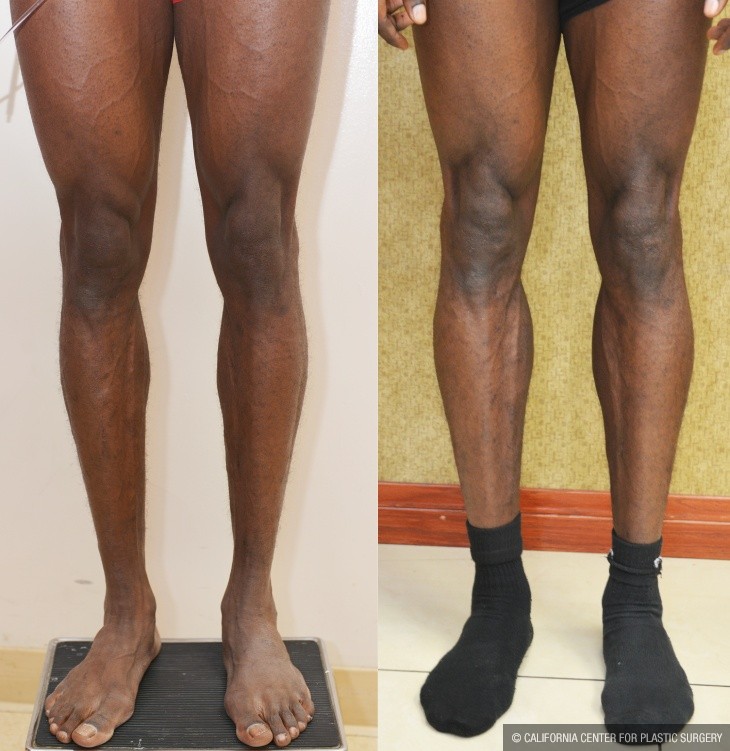
Calf Augmentation
Consultations offered at our three convenient locations in Encino, Glendale and Bakersfield
Contents
The Procedure
 Calf augmentation Beverly Hills is a cosmetic surgery procedure designed to enhance the appearance of the calves, enlarge them, and to make them more proportional in size and shape to the rest of the lower extremity and body. In this procedure calf implants of a variety of shapes, sizes, and contours, are inserted over the existing calf muscles — Gastrocnemius and Soleus Muscles — to achieve fuller and shapelier calves.
Calf augmentation Beverly Hills is a cosmetic surgery procedure designed to enhance the appearance of the calves, enlarge them, and to make them more proportional in size and shape to the rest of the lower extremity and body. In this procedure calf implants of a variety of shapes, sizes, and contours, are inserted over the existing calf muscles — Gastrocnemius and Soleus Muscles — to achieve fuller and shapelier calves.
The popularity of calf augmentation Beverly Hills among both men and women has soared in recent years as people are becoming more aware of the existence of this cosmetic surgery procedure. I am frequently told by consulting patients that, “If I knew that there was such a procedure to augment my calves with implants, I would have done it years ago.”
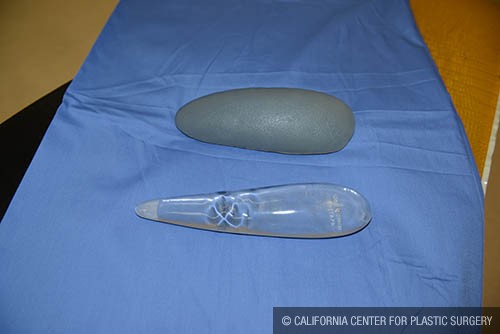
 Calf implants that are used for Calf Augmentation/ Enlargement are made of solid, rubberized silicone materials that have the consistency and firmness of muscle. They do come in a variety of sizes, shapes, contours, and surface textures.
Calf implants that are used for Calf Augmentation/ Enlargement are made of solid, rubberized silicone materials that have the consistency and firmness of muscle. They do come in a variety of sizes, shapes, contours, and surface textures.
Unlike silicone breast implants, calf implants are solid and don’t leak. The desired shape and size used depends on your existing form, goals, and physical limitations. Obviously, only implants that can safely fit in your legs can be used. The trend is to use longer implants that continue from 2 inches below the knee to 3-4 inches above the ankles. Older implants were usually shorter and made the legs look like “drum sticks” with lack of fullness in the lower leg. Older implants were also harder and did not have an anatomic shape. Today’s implants are softer, longer, and have an anatomic shape, unlike the cigar-shaped older implants.
Usually, two implants are used in each leg, in order to match the anatomic shape of the Gastorcnemius muscle which has two bellies. If one belly is much less developed than the other, then different size implants would be used to correct this asymmetry.
“I used to play football in college, and I always had a buff body, except for my skinny legs. Finally, I got the courage to do something about them. I wish I had gotten my calf implants sooner!” — George, age 54
Benefits
“I always thought that only bodybuilders get their calves done, until I found that my friend had them done. They look very natural and sexy. Now she is always wearing skirts and showing off her legs. I am very happy for her and am considering having my calves augmented as well.” — Alma, age 32
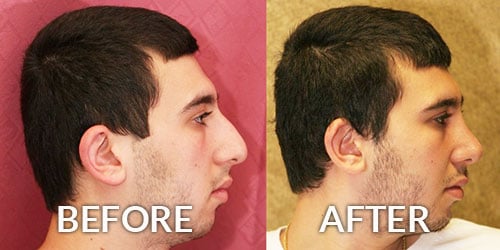
Men and women have different reasons for wanting to have their calves augmented. Men who work out and have a well-built upper body, often are ashamed of their “chicken legs” or “bow legs.” They are often frustrated by not being able to build-up their lower body and calves in proportion to their upper body. They also want to show off their “pumped” body in tank tops but feel uneasy about wearing shorts. On the other hand, there are those who seek calf augmentation Beverly Hills as a means of restoring calves that have lost volume as a result of congenital or physical defects such as Polio, Spina Bifida, and Club Feet.
The reason women get calf augmentation is to get curvaceous and sexy legs. This becomes more of an issue when they wear high heels, because the calves become most noticeable then. They want to show off their silky and smooth legs, which have all the right curves. It’s all about body language.
What’s Involved
The placement of calf implants usually involves a similar procedure, although each procedure requires a high level of expertise to place the implants correctly. During your consultation, Dr. Younai will usually measure your calves in order to help determine the appropriate size of your implants. Calf augmentation surgery is usually performed under general anesthesia. The implants are inserted through incisions in the back of the knees. Both the skin and the fascia – the fibrous material covering the muscle – are cut. A pocket is then created between the fascia and muscle in order to hold the implant. This pocket must be secure and able to hold the implant without moving. Implants can be used to enhance the appearance of the medial belly of the muscle, the lateral belly, or both. Once the implants are placed and inspected, the incisions are closed.
Aesthetic Goals
I always avoided wearing shorts or going to the pool with friends because of my ‘chicken legs.’ No matter how hard I worked out, I just couldn’t develop my calves. After calf augmentation, I am no longer self-conscious about my calves.” — Joe, age 34
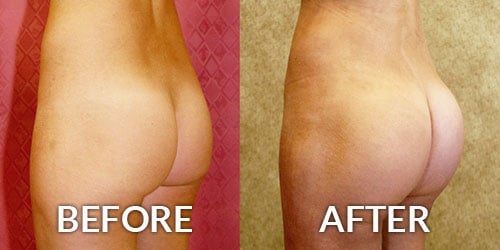
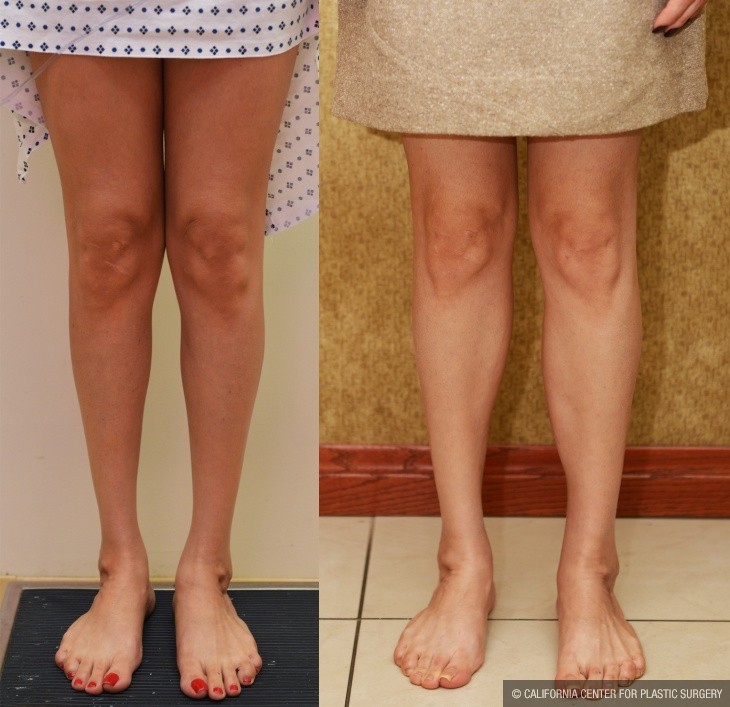
Most people want their calves to look natural, full, and curvaceous. In many men, the overwhelming emphasis is to augment the size and bulk of the calves in order to make them look as if you have worked out. Looking at the legs from the front, the medial (inner) belly of the Gastrocnemius muscle needs to look full-bodied and strong. Looking from the side, the Lateral (outer) belly of the Gastrocnemius muscle is mostly visible, and its augmentation contributes to forming the curve and flow of the leg. In women, this feature is usually more important, but the ultimate goal is to achieve a natural balance.
Before and After Photos
Preparation
Your surgeon will provide very specific instructions prior to surgery so you will have an optimal and safe experience. These include what medications to avoid to prevent excessive bleeding and bruising, required medical exams, what to eat and drink prior to surgery, and the prescription of an anti-nausea pill to take on the morning of the surgery.
In all cases, you will be asked to have a reliable friend or family member take you home after the surgery, as you will not be allowed to drive.

- You need to obtain comfortable shoes that have heels. Men usually wear boots with higher heels. Heels reduce the stretch on the calf muscles during recovery.
- Also obtain a walker or a cane to support your ambulation for the first week after surgery. Because of the stretching and aching of the calf muscles, you will not be steady on your feet during this time, and therefore a walker or cane is most helpful.
- Tend to all of your chores and do things before your surgery so you don’t have to worry about taking care of things early during your recuperation. You are not allowed to engage in heavy lifting for several weeks after surgery. This means if you should make arrangements for someone to help you with your heavy lifting chores for two weeks after surgery.
- Have your hair cut, pay your bills, and take your dog to the vet before your planned day of surgery!
- If you an avid tanner, don’t tan your legs for two weeks before, and six weeks after, your surgery. Any sun or tan burn of your leg skin can potentially increase the risk of having permanent scarring.
- If you routinely have your leg hair removed by shaving or waxing, avoid doing this for one day prior to, and three weeks after, surgery. Any trauma or nick to the leg skin during the early phase of healing can potentially increase the chance of developing an infection.
- If you are planning to have any procedure done to your legs, such as sclerosis of the leg veins or spider veins, please postpone this until after your legs have completely healed.
- Rent your favorite movies, and leave easily prepared foods and snacks in areas where you will not have to lift or reach.
- Place all of the medications, tissues, reading materials, water bottles on one table, within easy reach.
- Have ice cold cola drinks, ginger ale, or sport drinks close to your bed. Avoid drinking too much plain water after surgery, because it makes you more nauseated.
- After surgery take your nausea pill about one hour before your other medications to lessen nausea. Also, have some over-the-counter anti-acids available at your bedside.
- Some surgeons recommend putting cold packs on your calves afterwards. In my opinion, even though cold might lessen the inflammation, it can also cause frostbites or skin damage while your calves are numb after surgery.
- Arnica Montana or Bromelain homeopathics herbs have been used in Europe for centuries to treat swelling, soreness and bruising. When properly prepared, Arnica may significantly decrease the healing time or the appearance of such. There are many formulations from different companies. Sublingual (under the tongue) types are the most often recommended for plastic surgery. I have seen variable results with its use. There are some patients who did not benefit from it and others who appeared to benefit. Therefore, I am open to its use if a patient would like to use i
Pre-Operative Checklist
- If you are older than 45 years, or have heart disease, we require a pre-operative EKG, which would either be done by your internist, cardiologist, or at our facility. Heart disease and all other medical illnesses need to be monitored first by an internist or specialist.
- If you are anemic, or have a low blood count, please notify our office well in advance of surgery so that we can start you on an Iron supplement.
- Pre-operative laboratory blood and urine tests are done usually within 10 days of your surgery date. If you do have health insurance this might be covered, otherwise, the laboratory will charge you.
- If you have specific medical illnesses, allergies, or physical handicaps, please notify our staff during your pre-operative visit.
- Please refrain from taking any Aspirin, Aleve, Advil, Motrin or other NSAID for ten days before your surgery. These drugs can increase the incidence of bleeding and bruising.
- Do not drink or eat after midnight, the night before your surgery. This means no coffee or breakfast in the morning of your surgery. You should take all your medications with a little water.
- Please remove and leave behind all jewelry, watches, and body rings before you come in for your surgery. Please do not wear any makeup, body lotion, or perfume.
- Before leaving home for your surgery, take one “nausea pill”- COMPAZINE – with a little water.
- Please wear comfortable and loose clothing the day of surgery. It would be helpful if you wear front open tops and loose sweat pants. Also, bring your comfortable shoes with heels.
- You should make arrangements for a responsible adult friend or family member to take you home after surgery. You are not allowed to drive yourself home or take a taxi. After surgery, this caregiver is required to stay with you and to monitor and assist you for at least the first 24 hours after surgery. If you don’t have such a person please let us know in advance so that we can help you make arrangements for a stay at an after-care facility or hospital.
Having a support system of family, friends or a professional caregiver in the days following surgery is of the utmost importance, as the patient will need assistance with everyday tasks, such as going to the bathroom.
Recovery
After surgery, you are monitored in the recovery room by nurse. During this time your legs are kept elevated over a few pillows. You would most likely feel either nothing in your legs because of the local anesthetics or a pain which is similar to leg cramps.
 Before discharging you to go home, the recovery room staff will have performed safety checks on your legs, and have instructed your caregivers about your needs.
Before discharging you to go home, the recovery room staff will have performed safety checks on your legs, and have instructed your caregivers about your needs.
When patients leave the surgery facility to go home, they are usually groggy for about 12 hours or overnight. That is why it is very important to have someone who can assist you with getting around and taking your medications for at least the first 24 hours.
Instructions
- Make sure that you have all your medications, cold drinks, and towels at your bedside.
- Most people are nauseated during the first 24-48 hours. To reduce this, we suggest that you take your nausea pill one hour before taking your pain pills or antibiotics. While it is good to drink plenty of liquids, please refrain from drinking plain water or acidic fruit juices because they will make you more nauseated.
- Have your caregiver and/or yourself check the sensation and mobility of your feet, periodically during the first day. If there is any deterioration in circulation, sensation, or the patient’s ability to feel touch over his/her leg, please report this to your surgeon immediately.
- Patients will feel muscle cramp pain, pressure, and tightness of the calves which is relieved by prescription narcotics.
- Antibiotics are prescribed to reduce the risk of infection. Take your antibiotics and pain medications with food to lessen the chance of nausea.
- It is good to periodically move your toes and feet to increase circulation and to reduce your risk of forming blood clots.
- There will be some swelling and some minimal bruising which dissipates five to eight weeks following surgery. However, you should wait to buy new clothing until your size has stabilized.
 Following calf augmentation surgery, your legs are placed in a compression garment that covers your knee and calves. Do not remove this until your doctor instructs you to do so. We usually have the patient remove their bandages and to take a shower after 2 days. The incision sites and sutures can get wet in the shower. After showering, blow dry the paper strips over the incisions. Apply Vaseline or heavy lotion all over calves and legs, but not over the paper strips that cover your incisions. You should touch your legs, but don’t massage these areas deeply for about six weeks. Sometimes, patients whose skin was not firm and elastic will experience dimpling or wrinkling of the skin. These can be eliminated or minimized by gentle massaging over time.
Following calf augmentation surgery, your legs are placed in a compression garment that covers your knee and calves. Do not remove this until your doctor instructs you to do so. We usually have the patient remove their bandages and to take a shower after 2 days. The incision sites and sutures can get wet in the shower. After showering, blow dry the paper strips over the incisions. Apply Vaseline or heavy lotion all over calves and legs, but not over the paper strips that cover your incisions. You should touch your legs, but don’t massage these areas deeply for about six weeks. Sometimes, patients whose skin was not firm and elastic will experience dimpling or wrinkling of the skin. These can be eliminated or minimized by gentle massaging over time.- Some areas over the calves and the feet will remain numb for four to eight weeks. Massage will help to desensitize your skin in order to avoid hypersensitivity or skin irritation.
- When laying down or sitting, it is good to keep your legs elevated over several pillows, during the first week. Use your walker or cane to steady yourself during the first week.
- Most patients will have a two inch incision that will heal and become faint over 6-12 months.
- Avoid shaving and tanning of your legs for four weeks after surgery.
The support of your family and loved ones can be as important to your healing as following your physician’s medical directives. Their understanding of the pain, discomfort, and at times, the roller coaster of emotions, that you might experience can make all the difference in having an optimal outcome.
Suggestions

- You should be available as a full time caregiver for at least 24 hours to help the patient with the tasks that are normally taken for granted, like being able to walk to the bathroom.
- You, or someone, should care for the patient’s children for a minimum of two days, and be sure that she/he has assistance in lifting young children for several days after your surgery.
- Help with pet care. Someone should walk them, feed them and clean up after them for at least several days.
- The hardest task for the patient is walking and getting off the chair or bed during the first week. Help patients with these tasks.
- Prepare to help the patient address the swelling that he/she will experience, according to his physician’s instructions. This may include massaging the legs.
- Know that patient may experience mood swings, and feel irritable– especially in the first couple of weeks. This is a normal aftermath of major surgery.
- Encourage the patient to drink lots of water – to address bloating and to keep him hydrated.
- Remind the patient to not fight the pain – to go with the flow, and take his medications as directed. It is not good to try and be a hero!
- Give lots of compliments. He may be fearful because it will take some time before his legs appear as they should. He has a lot of healing to do!
- Prepare simple and easily digestible foods, such as scrambled eggs or Jello.
- Remind and reassure him that things will get better and less uncomfortable soon!
- Be there when he goes to have his bandages removed, to support him through any discomfort that he may be feeling.
- As far as sex is concerned, let the patient take the initiative.
- Some patients feel scared that they might harm their legs if touched or manipulated after surgery. Have him ask his doctor about this and get some reassurance.
- Some patients feel depressed or regretful about having undergone surgery. Sometimes they don’t know how to handle the attention or questions that a new appearance brings about. At the same time, significant others can develop uneasy feelings about the fact that you underwent such surgery. It is good to talk about your feelings and to even seek outside help if you can’t resolve some ambiguities.
Q & A
How Painful Is Calf Augmentation Surgery?
The immediate pain after calf augmentation feels like a leg cramp after working out hard. This pain is worst during the first 24-48 hours after surgery and can be managed with narcotic medication and leg elevation. Wearing shoes with heels takes the pressure off the calves when walking. Using a walker or cane during the first week also takes much pressure off the calves.
When Can I Resume Work and Exercise?
Most patients can resume relative normal activities in about seven days following calf augmentation. Most patients return to work in about a week.
You may resume upper body exercising within that time frame. However, you should resume activity only as is comfortable for you. For a period of three weeks, you should refrain from squatting, bending, and jogging because your muscles will be bruised. You may do calf exercises in about six weeks or when cleared by your plastic surgeon.
Will Calf Implants Limit Exercize
Calf augmentation does not hinder your ability to build up your leg and calf muscles. In fact, some doctors believe that after releasing the calf fascia your own calves have a better chance to grow with training.
When Can I Resume Sexual Relations?
Calf augmentation does not hinder your ability to have sexual relations. However, you should resume sexual activity only as you feel comfortable in doing so. The desire to resume having sex varies from patient to patient.
What If I get kicked in the Legs?
After you have completely healed, your calf implants are usually very sturdy and cannot get damaged by blunt trauma; unless you sustain a deep laceration of your leg directly over the implants.
Results Of Age?
Calf implants do not disintegrate over your lifetime and don’t have to be changed again. They usually maintain their form and looks with aging.
Risks & Complications
Every surgical procedure involves a certain amount of risk and it is important that you understand these risks and the possible complications associated with them. In addition, every procedure has limitations.
An individual’s choice to undergo a surgical procedure is based on the comparison of the risk to potential benefit. Although the majority of patients do not experience these complications, you should discuss each of them with your plastic surgeon to make sure you understand all possible consequences of calf augmentation. Problems associated with calf implants can be inherent to this type of implanted medical device or relate to complications of a surgical procedure. Additional advisory information regarding this subject should be reviewed by patients considering surgery that involves calf implants.
Bleeding
It is possible, though unusual, to experience a bleeding episode during or after surgery. Should post-operative bleeding occur, it may require emergency treatment to drain accumulated blood or blood transfusion. Intra-operative blood transfusion may also be required. Hematoma may contribute to capsular contracture, infection or other problems. Do not take any aspirin or anti-inflammatory medications for ten days before or after surgery, as this may increase the risk of bleeding. Non-prescription “herbs” and dietary supplements can increase the risk of surgical bleeding. Hematoma can occur at any time following injury to the legs, such as aggressive exercise or stretching, direct blows to the leg that can cause soft tissue or bony damage. If blood transfusions are necessary to treat blood loss, there is the risk of blood-related infections such as hepatitis and HIV (AIDS). Heparin medications that are used to prevent blood clots in veins can produce bleeding and decreased blood platelets.
Seroma
Fluid may accumulate around the implant following surgery, trauma or with vigorous exercise that was started early after surgery. Additional treatment may be necessary to drain fluid accumulation around calf implants. This may contribute to infection, capsular contracture, or other problems.
Infection
In general, surgeries of the lower extremities carry a higher chance of infection than those of upper extremities or trunk. Although infection is unusual after this type of surgery, it may appear in the immediate post-operative period or at any time following the insertion of a calf implant. Subacute or chronic infections may be difficult to diagnose. Should an infection occur, treatment including antibiotics, possible removal of the implant, or additional surgery may be necessary. Infections with the presence of a calf implant are harder to treat than infections in normal body tissues. If an infection does not respond to antibiotics, the calf implant may have to be removed. After the infection is treated, a new breast implant can usually be reinserted. It is extremely rare that an infection would occur around an implant from a bacterial infection elsewhere in the body, however, prophylactic antibiotics may be considered for subsequent dental or other surgical procedures. In extremely rare instances, life-threatening infections, including toxic shock syndrome have been noted after any implant surgery. Individuals with an active infection in their body or weakened immune system should not implant augmentation.
Scarring
All surgery leaves scars, some more visible than others. Excessive scarring can occur in people that are prone to Keloid or hypertrophic scar formation. Although good wound healing after a surgical procedure is expected, abnormal scars may occur within the skin and deeper tissues. Scars may be unattractive and of different color than the surrounding skin tone. Scar appearance may also vary within the same scar. Scars may be asymmetrical (appear different on the right and left side of the body). There is the possibility of visible marks in the skin from sutures. In some cases, scars may require surgical revision or treatment.
Pain
You will experience pain after your surgery. Pain of varying intensity and duration may occur and persist after calf implant surgery. Sever pain may be the result of improper implant size, placement, surgical technique, capsular contracture, compartment syndrome, or sensory nerve entrapment or injury. Chronic pain may occur very infrequently from nerves becoming trapped in scar tissue or due to tissue stretching.
Delayed Healing
Wound disruption or delayed wound healing is possible. Some areas of the leg skin incision may not heal normally and may take a long time to heal. This may require frequent dressing changes or further surgery to remove the non-healed tissue. Individuals who have poor circulation to their lower extremities, those with diabetes, those on steroids, and those that have had previous lower extremity surgery, trauma, or radiation, may be at increased risk for wound healing and poor surgical outcome. Smokers have a greater risk of skin loss and wound healing complications.
Skin Discoloration / Swelling Some bruising and swelling normally occurs after calf augmentation. The skin in or near the surgical site can appear either lighter or darker than surrounding skin. Although uncommon, swelling and skin discoloration may persist for long periods of time and, in rare situations, may be permanent.
Some bruising and swelling normally occurs after calf augmentation. The skin in or near the surgical site can appear either lighter or darker than surrounding skin. Although uncommon, swelling and skin discoloration may persist for long periods of time and, in rare situations, may be permanent.
Sutures
Most surgical techniques use deep sutures. You may notice these sutures after your surgery. Sutures may spontaneously poke through the skin, become visible or produce irritation that requires suture removal.
Implants
Calf implants, similar to other medical devices, can fail. Unlike silicone gel-filled breast implants, calf implants are made out of solid medical grade silicone which can not leak. Breakdown or fragmentation of a solid implant can occur as a result of an injury. Damaged implants require replacement or removal. Calf implants can wear out, they are not guaranteed to last a lifetime and future surgery may be required to replace one or both implants. A MRI (magnetic resonance imaging) study may be necessary to evaluate the possibility of implant fragmentation or breakdown, yet it may not be 100% accurate in diagnosing implant integrity.
Capsular Contracture
Scar tissue, which forms internally around the calf implant, can tighten and make the calves look round, firm, and possibly painful. Excessive firmness of the calf implants can occur soon after surgery or years later. The occurrence of symptomatic capsular contracture is not predictable. The incidence of symptomatic capsular contracture can be expected to increase over time. Treating capsular contracture may require surgery, implant replacement, or implant removal. Capsular contracture may reoccur after surgical procedures to treat this condition.
Implant Extrusion / Tissue Necrosis
 Lack of adequate tissue coverage or infection may result in exposure and extrusion of the implant through the skin. Tissue breakdown (necrosis) has been reported with the use of steroid drugs, after chemotherapy/radiation to the lower extremity tissue, due to smoking, microwave diathermy, sclerotherapy injections, skin burns, and excessive heat or cold therapy. In some cases, incision sites fail to heal normally. An implant may become visible at the surface of the calves as a result of the device pushing though layers of skin. If tissue breakdown occurs and the implant becomes exposed, implant removal may be necessary. Permanent scar deformity may occur.
Lack of adequate tissue coverage or infection may result in exposure and extrusion of the implant through the skin. Tissue breakdown (necrosis) has been reported with the use of steroid drugs, after chemotherapy/radiation to the lower extremity tissue, due to smoking, microwave diathermy, sclerotherapy injections, skin burns, and excessive heat or cold therapy. In some cases, incision sites fail to heal normally. An implant may become visible at the surface of the calves as a result of the device pushing though layers of skin. If tissue breakdown occurs and the implant becomes exposed, implant removal may be necessary. Permanent scar deformity may occur.
Skin Dimpling
Visible and palpable dimples or irregularities can usually be noted early after surgery, which usually resolve with time.
Implant Shifting or Displacement
It is possible for the implants to shift, move out of place, or show irregularities. This shifting of the implants can occur as a result of early aggressive exercise, external trauma to the implants, and/or manipulation. Therefore, it is prudent to follow your doctor’s instructions and not to start exercising or jogging too early. Additional surgery may be necessary to attempt to correct this problem. It may not be possible to resolve this problem once it has occurred.
Asymmetry
No two calves of a person are identical. There are natural differences between the shape, size, and the contour of the two calves. Although surgery aims to improve symmetry, it is never possible to achieve it completely. Additional surgery may be necessary to attempt improvement of asymmetry after a calf augmentation.
Implant Visibility
Although not common, you might be able to feel and even see the contour or the edge of the implant. This depends on how thin your leg skin is and how large the implants are.
Implant size
The nature of your leg’s soft tissue and bone structure can limit the size of a calf implant that could be placed safely. In order to go bigger, you might have to wait until your skin stretches with the first set of implants. At time it might not be even possible to place a too large of an implant.
Chronic Edema
In the immediate post-operative period there is normal edema or swelling of the legs. This usually dissipates over several weeks. People with history of poor circulation of their lower extremities are prone to the development of chronic or long term edema.
Compartment Syndrome Excessive swelling of the legs as a result of bleeding, edema, or pressure from the implants can cause an elevation in the pressure of the anterior (front) and/or posterior (back) compartments of the leg. If noted early and the pressure relieved by the removal of the implants, usually there are no long term consequence. Otherwise, there could be permanent damage to the muscles and nerves of the leg. Therefore, it is prudent that patients, caregivers, and medical staff report any unusual and abrupt increase in the post-operative pain, associated with increased numbness of the foot, and lack of mobility.
Excessive swelling of the legs as a result of bleeding, edema, or pressure from the implants can cause an elevation in the pressure of the anterior (front) and/or posterior (back) compartments of the leg. If noted early and the pressure relieved by the removal of the implants, usually there are no long term consequence. Otherwise, there could be permanent damage to the muscles and nerves of the leg. Therefore, it is prudent that patients, caregivers, and medical staff report any unusual and abrupt increase in the post-operative pain, associated with increased numbness of the foot, and lack of mobility.
Nerve Injury
Injury to the sensory nerves as well as motor nerve of the leg and foot is possible as a result of direct damage, increased pressure, and/or compartment syndrome. It is normal to experience some numbness and/or tingling of parts of the leg and foot after surgery. This is not alarming, is caused by general swelling, and usually dissipates over several months. On the other hand, rarely there could be direct injury to the common and lateral Popliteal Nerve which can cause a “foot drop”. According to reports in the literature this is usually reversible. Other nerve such as the Tibial or the Seural Nerve could also be injured, but this is very rare.
Surface Contamination of Implants
Skin oil, lint from surgical drapes, or talc may become deposited on the surface of the implant at the time of insertion. The consequences of this are unknown.
Unusual Activities and Occupations
Activities and occupations that have the potential for trauma to the calf implants could potentially break or damage calf implants or cause bleeding/Seroma.
Surgical Anesthesia
Both local and general anesthesia involve risks. There is the possibility of complications, injury, and even death from all forms of surgical anesthesia or sedation.
Allergic Reactions
In rare cases, local allergies to tape, suture material and glues, blood products, topical preparations or injected agents have been reported. Serious systemic reactions including shock (anaphylaxis) may occur in response to drugs used during surgery and prescription medicines. Allergic reactions may require additional treatment.
Thrombosed Superficial Veins
Thrombosed superficial veins, which resemble cords, occasionally develop in the area of the legs and knee and usually resolve without medical or surgical treatment.
Deep Venous Thrombosis and Pulmonary Embolism
With any surgery, especially those that involve the lower extremities, there is a chance of developing blood clots in the leg veins. Those who remain very inactive after surgery, or have had a history of deep venous thrombosis (DVT) are at a higher risk of developing DVT. Such blood clots can dislodge and travel to the lungs and heart. This is a serious event that can even cause death.
Cardiac and Pulmonary Complications
Pulmonary complications may occur secondarily to both blood clots (pulmonary emboli), fat deposits (fat emboli) or partial collapse of the lungs after general anesthesia. Pulmonary emboli can be life-threatening or fatal in some circumstances. Inactivity and other conditions may increase the incidence of blood clots traveling to the lungs causing a major blood clot that may result in death. It is important to discuss with your physician any past history of swelling in your legs or blood clots that may contribute to this condition. Cardiac complications are a risk with any surgery and anesthesia, even in patients without symptoms. Should any of these complications occur, you may require hospitalization and additional treatment. If you experience shortness of breath, chest pains, or unusual heart beats after surgery, seek medical attention immediately.
Damage to Deeper Structures
There is the potential for injury to deeper structures including nerves, blood vessels, muscle, joint, and bone during this surgical procedure. The potential for this to occur is rare. Injury to deeper structures may be temporary or permanent.
Shock
In rare circumstances, your surgical procedure can cause severe trauma, particularly when multiple or extensive procedures are performed. Although serious complications are infrequent, infections or excessive fluid loss can lead to severe illness and even death. If surgical shock occurs, hospitalization and additional treatment would be necessary.
Large Size Calf Augmentation
Patients who request an outcome of calf augmentation that produces disproportionately large calf size must consider that such a choice can place them at risk for a less than optimal long-term outcome and the need for re-operation and additional expenses. The placement of excessively-sized calf implants that exceed the normal dimensions of the legs produces irreversible tissue thinning, implant drop out, and visible/palpable rippling.
Mental Health Disorders and Elective Surgery
It is important that all patients seeking to undergo elective surgery have realistic expectations that focus on improvement rather than perfection. Complications or less than satisfactory results are sometimes unavoidable, may require additional surgery and often are stressful. Please openly discuss with your surgeon, prior to surgery, any history that you may have of significant emotional depression or mental health disorders. Although many individuals may benefit psychologically from the results of elective surgery, effects on mental health cannot be accurately predicted.
Unsatisfactory Result
Although good results are expected, there is no guarantee or warranty expressed or implied, on the results that may be obtained. You may be disappointed with the results of surgery. Asymmetry in implant placement, displacement, unanticipated calf shape and size, loss of function, wound disruption, poor healing, and loss of sensation may occur after surgery. Calf size may be not optimal. Unsatisfactory surgical scar location may occur. In some situations, it may not be possible to achieve optimal results with a single surgical procedure. It may be necessary to perform additional surgery to improve your results, change implant size or remove and not replace implants.
Calf Implant Technology / Technologic Improvements in Calf Implants
The technology of Calf implant design, development and manufacture will continue to progress and improve. Newer or future generations of implants may be better in some way from those currently available.
Female Patient Information
It is important to inform your plastic surgeon if you use birth control pills, estrogen replacement, or if you suspect that you are pregnant. Many medications including antibiotics may neutralize the preventive effect of birth control pills, allowing for conception and pregnancy.
Medications
There are potential adverse reactions that occur as the result of taking over-the-counter, herbal, and/or prescription medications. Be sure to check with your physician about any drug interactions that may exist with medications that you are already taking. If you have an adverse reaction, stop the drugs immediately and call your plastic surgeon for further instructions. If the reaction is severe, go immediately to the nearest emergency room. When taking the prescribed pain medications after surgery, realize that they can affect your thought process and coordination. Do not drive, do not operate complex equipment, do not make any important decisions, and do not drink any alcohol while taking these medications. Be sure to take your prescribed medication only as directed.
Smoking, Second-hand Smoke Exposure, Nicotine Products (Patch, Gum, Nasal Spray) Patients who are currently smoking, use tobacco products, or nicotine products (patch, gum, or nasal spray) are at a greater risk for significant surgical complications of skin dying and delayed healing. Individuals exposed to second-hand smoke are also at potential risk for similar complications attributable to nicotine exposure. Additionally, smoking may have a significant negative effect on anesthesia and recovery from anesthesia, with coughing and possibly increased bleeding. Individuals who are not exposed to tobacco smoke or nicotine-containing products have a significantly lower risk of this type of complication. Please indicate your current status regarding these items below:
Patients who are currently smoking, use tobacco products, or nicotine products (patch, gum, or nasal spray) are at a greater risk for significant surgical complications of skin dying and delayed healing. Individuals exposed to second-hand smoke are also at potential risk for similar complications attributable to nicotine exposure. Additionally, smoking may have a significant negative effect on anesthesia and recovery from anesthesia, with coughing and possibly increased bleeding. Individuals who are not exposed to tobacco smoke or nicotine-containing products have a significantly lower risk of this type of complication. Please indicate your current status regarding these items below:
Health Insurance
Most health insurance companies exclude coverage for cosmetic surgical operations such as a calf augmentation or any complications that might occur from surgery. Please carefully review your health insurance subscriber-information pamphlet. Most insurance plans exclude coverage for secondary or revisionary surgery due to complications of cosmetic surgery.
Financial Responsibilities
The cost of surgery involves several charges for the services provided. The total includes fees charged by your surgeon, the cost of surgical supplies, anesthesia, laboratory tests, and possible outpatient hospital charges, depending on where the surgery is performed. Depending on whether the cost of surgery is covered by an insurance plan, you will be responsible for necessary co-payments, deductibles, and charges not covered. The fees charged for this procedure do not include any potential future costs for additional procedures that you elect to have or require in order to revise, optimize, or complete your outcome. Additional costs may occur should complications develop from the surgery. Secondary surgery or hospital day-surgery charges involved with revision surgery will also be your responsibility. You may be advised some time in the future to have a MRI (magnetic resonance imaging) scan to determine the condition of your implants. You would be responsible for future costs of such imaging studies. In signing the consent for this surgery/procedure, you acknowledge that your have been informed about its risk and consequences and accept responsibility for the clinical decisions that were made along with the financial costs of all future treatments.